Diverticula are pockets that develop in the colon wall, usually in the sigmoid or left colon, but may involve the entire colon. These small pouches bulge outward through weak spots in the colon wall. Each pouch is called a diverticulum. Multiple pouches are called diverticula. The condition of having diverticula is called diverticulosis. About 10 percent of Americans older than 40 have diverticulosis. The condition becomes more common as people age. It affects about 50% of Americans by age 60, and nearly 100% by age 80.
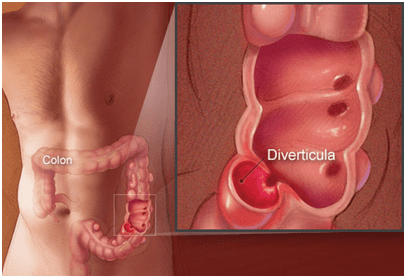
Diverticulosis describes the presence of these pockets, while diverticulitis, an infection of the pockets, describes inflammation or complications of these pockets.
Diverticula are most common in the lower portion of the large intestine, called the sigmoid colon. When the pouches become inflamed, the condition is called diverticulitis. Ten to 25 percent of people with diverticulosis get diverticulitis.
 Infection can lead to complications, such as swelling or rupturing of the diverticula, abscesses, bowel blockage, or leaks through the bowel wall. If one of the pouches becomes infected and inflamed, bacteria may enter small tears in the surface of the bowel, leading to small abscesses. In rare cases, the infection spreads and breaks through the wall of the colon causing infection or abscesses in the abdominal cavity. Such infections are very serious and can be life threatening unless treated without delay.
Infection can lead to complications, such as swelling or rupturing of the diverticula, abscesses, bowel blockage, or leaks through the bowel wall. If one of the pouches becomes infected and inflamed, bacteria may enter small tears in the surface of the bowel, leading to small abscesses. In rare cases, the infection spreads and breaks through the wall of the colon causing infection or abscesses in the abdominal cavity. Such infections are very serious and can be life threatening unless treated without delay.
Causes, incidence, and risk factors
No one knows exactly what causes the sacs, or pouches of diverticulosis to form. Eating a low-fiber diet is one of the most likely causes. The disease was first noticed in the United States in the early 1900s, around the time processed foods were introduced into the American diet. Consumption of processed foods greatly reduced Americans’ fiber intake.
People, who eat mostly processed food, as many Americans eat, do not get enough fiber in their diet. Processed foods include white rice, white bread, most breakfast cereals, crackers, and pretzels.
Diverticular disease is common in developed or industrialized countries—particularly the United States, England, and Australia—where low-fiber diets are consumed. The disease is rare in Asia and Africa, where most people eat high-fiber diets. Fiber is the part of fruits, vegetables, and grains that the body cannot digest. Some fiber, called soluble fiber, dissolves easily in water. It takes on a soft, jelly-like texture in the intestines. Insoluble fiber passes almost unchanged through the intestines. Both kinds of fiber help prevent constipation by making stools soft and easy to pass.
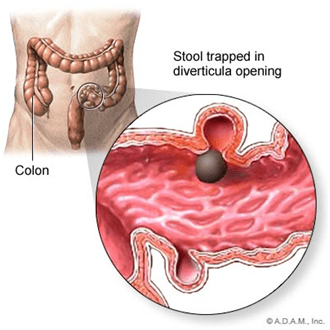
Diverticulosis is very common. It is found in more than half of Americans over age 60. Only a small number of these people will develop diverticulitis.
Doctors are not certain what causes diverticula to become inflamed. The inflammation may begin when bacteria or stool are caught in the diverticula. An attack of diverticulitis can develop suddenly and without warning.
Symptoms
Most people with diverticulosis do not have any discomfort or symptoms, but they may have bloating and cramping in the lower part of the belly.
Symptoms of diverticulitis are more severe and often start suddenly, but they may become worse over a few days. The most common symptom of diverticulitis is abdominal pain. The most common sign is tenderness around the left side of the lower abdomen. If infection is the cause, fever, nausea, vomiting, chills, cramping, and constipation may occur as well. The severity of symptoms depends on the extent of the infection and complications.
Diverticulitis Diagnostic Tests
A CT scan is generally the best test to diagnose diverticulitis. Diverticulosis is usually diagnosed on routine colonoscopy.
Treatment
The treatment of diverticulitis depends on the severity of your symptoms. Some people may need to be hospitalized, but most patients can be treated at home with antibiotics.
At home treatment usually includes oral antibiotics, dietary restrictions, and possibly, stool softeners. Eating a high-fiber diet is sometimes the only treatment necessary.
Once these pouches have formed, you will have them for life. If you make a few simple changes in your lifestyle, you may not have diverticulitis again.
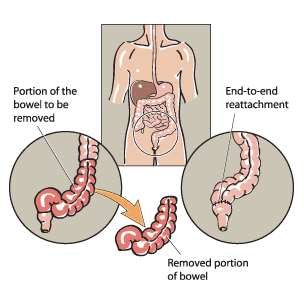
Surgery is required only when complications occur, attacks keep recurring, or when people have severe attacks with little response to medication. Surgery for diverticular disease can be performed by laparoscopic or minimally invasive techniques. Surgery involves removing part of the colon, usually the sigmoid colon, and reattaching it to the rectum.
Complications of Diverticulitis
Diverticulitis can lead to bleeding; infections; small tears, called perforations; or blockages in the colon. These complications always require treatment to prevent them from progressing and causing serious illness.
 Bleeding
Bleeding
Rectal bleeding from diverticula is a rare complication. Doctors believe the bleeding is caused by a small blood vessel in a diverticulum that weakens and then bursts. When diverticula bleed, blood may appear in the toilet or in the stool. Bleeding can be severe, but it may stop by itself and not require treatment. A person who has bleeding from the rectum—even a small amount—should see a doctor right away. Often, colonoscopy is used to identify the site of bleeding and stop the bleeding. Sometimes the doctor injects dye into an artery—a procedure called angiography—to identify and treat diverticular bleeding. If the bleeding does not stop, surgery may be necessary to remove the involved portion of the colon.
Abscess, Perforation, and Peritonitis
Diverticulitis may lead to infection, which often clears up after a few days of treatment with antibiotics. If the infection gets worse, an abscess may form in the wall of the colon.
An abscess is a localized collection of pus that may cause swelling and destroy tissue. If the abscess is small and remains in the wall of the colon, it may clear up after treatment with antibiotics. If the abscess does not clear up with antibiotics, a radiologist may need to drain the abscess by inserting a catheter—a small tube – into the abscess through the skin. This process may be guided with the help of a CT scan.
Infected diverticula may lead to a perforation of the colon. In these cases, the perforations leak pus and stool out of the colon into the abdominal cavity, a condition called peritonitis. A person with peritonitis may be extremely ill with nausea, vomiting, fever, and severe abdominal tenderness. The condition requires immediate surgery to clean the abdominal cavity and remove the damaged part of the colon. Without prompt treatment, peritonitis can be fatal.
Fistula
A fistula is an abnormal connection of tissue between two organs or between an organ and the skin. When damage, infected tissue comes into contact with normal tissue during an infection, they sometimes stick together. If they heal that way, a fistula may form. When diverticulitis-related infection spreads outside the colon, the colon’s tissue may stick to nearby tissues. The organs usually involved are the bladder, small intestine, and skin.
The most common type of fistula occurs between the bladder and the colon. This type of fistula affects men more often than women. It can result in a severe, long-lasting infection of the urinary tract. The problem can be corrected with surgery to remove the fistula and the affected part of the colon.
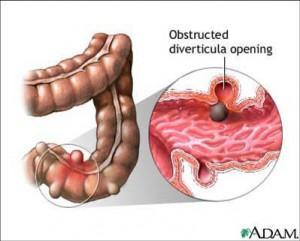
Intestinal Obstruction
Scarring caused by infection may lead to partial or total blockage of the intestine, called intestinal obstruction. When the intestine is blocked, the colon is unable to move bowel contents normally. If the intestine is completely blocked, emergency surgery is necessary. Partial blockage is not an emergency, so the surgery to correct it can be planned.
Laparoscopic Colon Resection
A technique known as minimally invasive laparoscopic colon surgery or resection allows surgeons to perform many common colon procedures through small incisions. Depending on the type of procedure, patients may leave the hospital in a few days and return to normal activities more quickly than patients recovering from open surgery.

 Bleeding
Bleeding